CLAUDIU IONESCU
talking to
Acad. Prof. Dr. IRINEL POPESCU
on his anniversary of 70 years old

Towards the end of 1997 I became the Secretary of the “Phoenix” Lodge of the NGLR, and the Orator of the Lodge was Professor Irinel Popescu, founding father in the field of top-class medicine. Exactly twenty years ago, the Professor granted me an interview in the “Masonic Forum” Magazine. With people of his calibre, Universal Masonry gained identity and established itself as an elite initiation structure. Irinel Popescu is a builder by calling.
Professor, you recently turned 70 years old – a lifetime dedicated to saving human lives, a lifetime dedicated to study, with countless hours in the operating room. May you be healthy, Professor, and may you bring health to your patients! Many happy returns!
Thank you very much. I wish the very same to you and to all our viewers.

Thank you. As a professor, a member of the Academy, the director of a medical centre and top surgeon, you have a general overview of Romanian medicine and are a voice with undisputable authority and experience. Can you tell us, broadly speaking, what are its strong points and weak points?

With your permission, I would start with a quip that might be a bit inappropriate, but I have no reservations in saying it. I heard from an old radiologist who’d been an athlete in his youth. He would tell us about the famous football player Petschovschi, who before every game would tell the owners: “I know how to play football worth 500 lei and I know how play worth 2000 lei”. So medicine is a sector, like many others – maybe even more so –, dependant upon budget. The budget in Romania is as you know it, that is, by comparison, among the last in the EU. So we can’t have too high demands. Under these circumstances, there are, however, some strong points coming from several factors. One of them is tradition. Romanians have had a tradition of the medical school since the 19th century, with professors who’d studied in Paris and returned to do great deeds – not all of them succeeded, but that’s another story. Another one is a certain professional ego. I know plenty of professionals who, despite the conditions, sometimes against all odds directly concerning them, and with many sacrifices, really wanted to do something. Some of them actually did. That is why Romanian medicine still responds promptly, and in good fashion, to a desire stemming, maybe, from local mentalities: in the subconscious of the Romanian patient there is the conviction that they must be solved very quickly. The idea of a waiting list is common in Canada and other countries, sometimes the waiting takes months, maybe even a year. The Romanian patient doesn’t have patience, they need to be solved quickly. I would say that the majority of them indeed are solved quickly, to the limit of the Romanian system’s ability to do so. Most of them are solved well.
Some of the leaders of opinion in Romanian medicine are very well integrated in international circuits, they lecture at many international gatherings, they are considered authorities in the field and their ambition is to perform at the same level as their colleagues in the West, whom they always meet at congresses and take as a standard and as a term of comparison. Some of them, indeed, manage to do so. This has ramifications in a downward direction as well, throughout the network: interns learn in centres like these with professors such as these and so, overall, there are some strong points, both in terms of how quickly the issues are solved, quite often, and also in terms of the quality of the solutions. There are also weak points, with regards to the speed with which things are put in motion, and we come back to the budget issue. Technologies are changing very fast, generations of equipment are changing very fast. Sometimes, I admit, there is an “industry driven” tendency, which means listening to the interests of the industry in adopting new technologies. Maybe the typical example is the surgical robot. We can’t overlook this, we can’t refuse to align to current standards. Remember laparoscopy at first – it was viewed as something of a luxury. Today, nobody does open cholecystectomy anymore, it would be inconceivable to not have a laparoscopy. So there are some weak points, again, connected to an insufficient budget, there is not point avoiding this reality.
Unfortunately, countries like Romania have become markets for goods produced in developed countries and, at the same time, an exporter of experts. Romania is witnessing a large exodus of medics. Romanian academia has become a nursery for experts who are going abroad, but educated on the expense of the Romanian state. Add to this the fact that Romanian universities have faculties that teach in foreign languages, which creates the conditions for the bleeding of experts abroad. As a professor, as a medical trainer, what’s your opinion on this?
The fact that young people from other countries are educated here is a plus, they do not belong to Romanian medicine, they go back to where they came from. I wouldn’t say they are a bother, on the contrary, they offer added value to the Romanian school of medicine. So as not to exaggerate the bleeding of brains out of Romania, there probably is a hidden tendency of Romanian faculties to lower their level so much that our youth aren’t competitive abroad anymore. That’s probably the main reason for this, to stop the bleeding. But, jokes aside, let’s not dramatize.
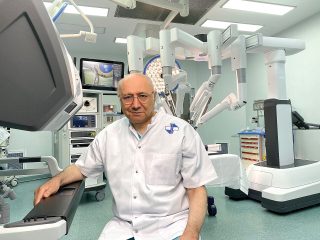
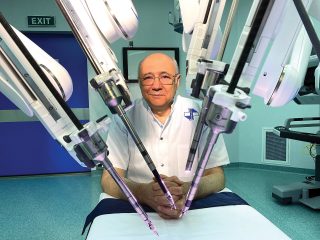
There are countries with a higher level than Romania where emigration is a known phenomenon. I would take Italy as an example. In the three years I spent in the United States I had many Italian colleagues, the majority of which remained there. The phenomenon is well-known, I don’t know to what extent it continues to this day, but over the years it was obvious. Nobody complained because of it. There are enough young people who remain here as well, some of them very gifted. On the other hand, even with this quote-unquote “bleeding of the brains”, it is increasingly harder to obtain a position in Romanian medicine. The positions open now are fewer than before. Access to some positions in big hospitals and large university cities is a lot more difficult, so that says something as well. A few years ago, at a “Solomon Marcus” Conference, I said something based on what the late member of the Academy had stated, that we should stop dramatizing and start shifting the paradigm with regards to the exodus of the brains, while at the same time trying to capitalize on the very important positions some of the members of the diaspora have obtained. This is something that happens continuously, because there is no category more willing to help Romania, to bring Romania to the highest level of knowledge and technology, than the Romanian diaspora. So, on the one hand, we are sorry that these young people have left, on the other we have to stay close to them and they to us and bring the highest level of medicine back here, home, with their help. This does happen. I know plenty of examples. Sometimes there is a win-win situation, because some of them, who are in very high positions abroad, bring gifted – even overgifted, I would say – young people from Romania and use them as work force – of course, cheaper than the workforce on the specific market –, and with results that are sometimes much better.
The prosaic truth is that a surgeon generally can’t have feelings during the operation. He mustn’t allow himself to be overwhelmed by fear, panic, by the idea that the patient’s life is in his hands. What do you feel in the operation room when you know that everything depends on you, on the precision of the surgical act and medical knowledge? Were you ever afraid? On the other hand, the power to bring someone back to life – I am a bit pathetic now –, to fix what isn’t working right in the human body: doesn’t it make you feel a bit different, above the rest, superior, like a little God?
No, no, to start from the end – absolutely not, this is the cut and clear answer. It would be a huge mistake and an entirely faulty professional approach. Coming now to the first part of the question, during an operation you don’t really have time to think outside of the operative times, the operative gestures, the lesion you have to fix. Often times you don’t even have time to be afraid. I have to admit that when I started as a transplantologist I would feel a certain fear after I would take out the sick liver and have in front of me an empty hepatic fossa, knowing that if the new liver isn’t implanted very quickly and doesn’t work properly that patient is a dead man. This creates a sense of anxiousness, because when you do resections and reconstructions you really have time to think only about the lesion and what you are doing. When you have a hepatic fossa in front of you that’s missing an organ and you have to replace it quickly and on time, and it has to start working immediately, there comes a certain sense of fear which takes a while to overcome.

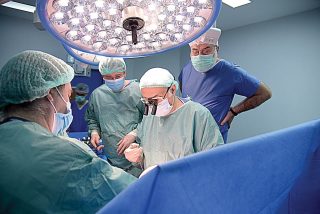
Do you have a ranking of the surgeries you’ve performed? The most difficult, the longest, the most demanding?
No, I don’t. I have an admiration for my colleagues who report tens of thousands of surgeries. This isn’t a job based on quantity, but on quality. At one point I would ask, for instance, roughly how many surgeries are done in each room in a big hospital and I was answered that it depends on the surgery. So it’s pointless to count, the number doesn’t say anything. There are surgeries that take 45 minutes to an hour, there are surgeries that take twelve hours – for instance, the liver transplant at its beginnings in Romania, in its pioneering stages. Back then I would harvest the liver from the donor, come back with it, prepare it on the so-called “back table”, the operation table, for another hour, maybe more, then I would remove the sick liver of the receiver, after that I would implant the healthy liver from the donor. That could take over twelve hours, sometimes even closer to twenty-four, if you count the time spent traveling when the donor was in Oradea, Cluj or Târgu Mureș. You don’t count the hours here, hours are irrelevant, what is important is the result. A therapist, no matter if he is a surgeon, an internist or any other medical discipline, is judged by their results. Not by their speed, sometimes not even by the elegance of the execution, by the performance at the operation table, but by the results. At the end of the day, this is the only thing that matters. Earlier I used the phrase “industry driven” – medicine is a “patient driven” industry, the evolution is dictated by the patient, by their expectations and by the results obtained by the doctor. If the results are good, it doesn’t matter if the doctor is tall or short, fat or slim, super-educated or less educated. There are many personality profiles but, at the end of the day, what matters for the patient is the result.
You are the one who introduced robotic surgery in Romania. It’s an interesting paradigm because, basically, you perform a virtual surgery on a live patient who is at a distance and only interacts with a machine that is remotely – and precisely – controlled by the surgeon. Human interaction is almost zero. Since for most of us this is sci-fi, something absolutely fabulous, I want to ask you, Professor, to describe what happens in robotic surgery.
The current quote-unquote “robot” we have, Da Vinci – but there will soon be others on the market, in quite a significant number –, is a telemanipulator, it’s not a true robot. A true robot is something you wind up, you put it there and it sweeps the floor or does something by itself. The Da Vinci telemanipulator, inaccurately called a “robot”, allows the surgeon, who sits at the console, sees everything better and in 3D by having a significant magnification and can spot tiny details of the operative point, to perform surgery inside the patient. Like you said, the surgeon is at a distance. Usually, this distance is several meters away, in the operation room. The surgeon is in the same operation room, at the console, just like in laparoscopy, through those small incisions. Robotic surgery is a minimally invasive form of surgery, just like laparoscopy. The arms of the robot reproduce the surgeon’s gestures inside the patient. At the end of the day, the surgeon is the one operating, the one manipulating the instruments, the one performing the operative gestures. The surgeon is able to see better, sit more comfortably, especially during long operations, the back and the eyes don’t get tired anymore, and the robotic surgery instruments have a point with seven degrees of freedom that allows for great versatility. First – it allows access to very narrow spaces, such as the profound pelvis or the subdiaphragmatic region, and second – it allows for movements that almost entirely replicate the movements of the human hand, something which isn’t the case in laparoscopy. It’s a minimally invasive form of surgery, and the robot is still, for now, a telemanipulator. The robot of the future, however, will certainly be a true robot, a mechanical system to which, as is the case with the Da Vinci robot, a lot of informatics will be attached. Even now, the informatics that the Da Vinci robot is based on is at the same level of data processing and programming as before. AI is only in its initial stages, it’s almost not there in the case of the Da Vinci robot. In the robotic systems of the future there will be more AI. Elon Musk says he stopped the research, but I’m not sure to what extent he will be able to stop them. The AI of the future, together with robot-like mechanical systems, will be able to operate by itself. That will be a real robot, for which the surgeon, sadly, will no longer be needed. But now I have to come back to what I was saying earlier about the interest of the patient, because such a system will certainly obtain better results than surgeons currently do.
So, basically, AI will be leading the process.
Yes, absolutely, yes. Right now there is a lot of informatics in robotic systems too. After all, we are talking about a quantity of information that has to be collected about the patient’s lesion – for a gastric tumour, let’s say, where it’s localized, how spread it is, what resection margins we have to ensure, how much we have to extend the resection. The surgeon evaluates this information in their mind, processes it in their mind, makes decisions in their mind. We already know that the processing speed and capacity of AI systems (that have neural networks, this is what defines AI) surpass the performance of the human mind.
I know that in the beginning there was one liver harvested from a human donor who was in brain death, and after that one from a live patient. In the interview you gave me twenty years ago you told me that Thomas Starzl’s team was very seriously studying the possibility of genetically engineering pigs whose liver could be used in human transplants. That means that every patient with cirrhosis could electively benefit from a transplant operation – i.e. not wait for the death of a donor. The liver of every patient on the waiting list could be “produced” on demand according to the immunological characteristics and with the help of genetic engineering. Where are now in that regard?
Unfortunately, not very far from where we were twenty years ago. Some steps have been made and, from what I could observe about the evolution of medicine over the last almost fifty years, sometimes after these small accumulations there has been a breakthrough that led to finding the solution. Research is done on at least three fronts. One of them is what you said, xenostransplant, transplanting genetically modified organs from animals; genetically modified firstly in order to surpass the immunological barrier of the host which, as we know, exists in the case of human to human transplants too and requires post-operative immunosuppression. It is even stronger in the case of animal to human transplants and require special protocols and immunosuppression, as well as plasmapheresis, plus specific treatments in order to inhibit specific gene. These treatments haven’t had too much success so far. Over the years, xenotransplant has known periods of momentum, enthusiasm and very big expectations, then it fell off the radar, everything quiet, and then it reactivated. We are now in a period of reactivation, I would say, after the new procedures performed in Baltimore, which received quite a lot of press in Romania as well but in the end weren’t, unfortunately, successful. This is what happened in the 90’s as well, during the last part of my internship at Pittsburgh. Two liver transplants were made from baboon to humans. Both failed after a while, one of them faster, the other one later, but the patients didn’t survive. Then it was shut down. Now it’s been picked back up. The patient’s didn’t survive this time either. I don’t know if this is the path to success, we’ll see. A second way has to do with cells. Cell cultures have progressed a lot. From cell cultures – that is, in vitro cultivated hepatic cells – we have reached what are now called “organoids”, clusters of cells prefiguring the future organ, just as an embryo eventually reaches organogenesis; from a small bud an organ is eventually formed. This cell-organoid-organ connection is on the way, let’s say. It depends on how fast or slow we will reach the final stage, obtaining an organ starting from the cells. Lastly, the third way are the printed organs, and here we go back to informatics and AI – how capable is the AI of replicating all the characteristics of the hepatic cell and of the other cells forming the liver and then print an entire organ, an organ that can be used in a transplant. Again, it’s difficult for me to say how far or close we are from achieving this. Certainly, as I said, sooner or later one of these paths – or maybe a fourth one, which at the moment we can’t even suspect exists – will take us to a success. How soon or late this happens is very hard to predict because at some point, for example, with regards to xenotransplant, we thought we were very close, we thought we needed just a bit more for the problems to be solved and that in one or two years’ time we’d be there, we’d be able to transplant organs from animals. Actually, we found out it was sort of a morgana maiden, the closer we thought we got, the further it moved away from us.
By performing top medicine, liver transplants, robotic surgery you’ve certainly had very hard moments in your career. How did you manage to overcome them and not give in to hopelessness which is, after all, a very human feeling? At one time, in another interview, you said that the patients saved are quickly forgotten, while the unfortunate cases can’t be forgotten.
Yes, it’s true. I think the main reason to overcome such moments is the sense of duty towards all the other patients whom you actually have the duty to save, maybe precisely in memory of those you couldn’t. You have to see your mission through to the very end and, if we are to use a Christian analogy, bear your cross to the very end.
You’ve published something never seen before, outside the field of specialty literature while still having a strong connection to medicine, a book called The Life and Work of Professor Dan Setlacec. Here’s what you point out about it: “The book doesn’t claim to be an official biography, but rather the perspective of someone who has had the chance of directly knowing a great personality and feels it is his duty to testify”. Why a book about Professor Dan Setlacec?
On the one hand, out of a moral duty which, I think, every student has for their master, or at least should have. On the other, because I tried to follow a model, a model that wasn’t sufficiently used in Romanian “medicine memoir” literature, which in my case was Teodor Burghelea’s book about Nicolae Hortolomei, The Life and Work of Professor Nicolae Hortolomei. I consider this a standard model. Professor Burghelea wrote about his master’s life and work. You couldn’t really say who this book is for because the part called The Life can be read by anyone, whereas the part called The Work, which Burghelea copiously extended, describes complicated procedures and operations that only experts will understand. So you don’t really know who the book is for, but it has been a model. I was the type of person who tried to followed models as much as I could. I’ve always felt that if someone starts a tradition and that someone was validated as one of the leaders of Romanian medicine at the time, future generations have the duty to pick up that model. We don’t have anything left to invent, we don’t need to invent other models. On the other hand, we ourselves have the obligation of taking this tradition forward because, just as Burghelea wrote about Hortolomei and others have written about their masters, Ion Făgărășanu about Ernest Djuvara, but also other books following this model, so the current generation must show that it’s not a spontaneous generation, that it was trained in the school of certain masters, that in Romanian medicine there is a certain tradition which I touched upon in the beginning. So a moral obligation, in a way, and it carries on a model which I would want to see carried on as much as possible.
And the second part of the previous question, Professor: how important is the master-apprentice relationship? You have built things in medicine. Do you have professional apprentices?
Involuntarily! I don’t know if I can call them apprentices, I’m not sure if it’s the best term. The fact is that each of us, in a certain profession, forms some generations and, at a certain point, passes the torch to the next generation. If the members of the next generation see themselves as apprentices of the previous generation or not – that I do not know. I have seen individuals in Romanian medicine who are under the impression that medicine started with them. I don’t personally have a problem in that regard. I have tried to understand any sort of mentalities. Some have said that nothing their predecessors did was good and claim to have invented everything themselves. It would be normal to view this as a succession of generations and the most correct way would be to speak about the next generation, not necessarily apprentices, because some consider this to be too little – how could they be considered apprentices when some of them think they are the very top? It’s not the case with me and the school I founded at Fundeni, on the contrary, I’ve had the chance of training very good and very capable students. But I have seen in other places this idea that we don’t owe anything to our forebears and that the term “apprentice” is quite bothersome, that somehow everything starts with us, actually.
Professor, a question that appears in the set of any interview: how much time do you have for hobbies, for traveling, for anything else other than medicine? What hobbies does Irinel Popescu have, actually?
He doesn’t really have any hobbies anymore. I didn’t really have any, because I didn’t have time. And, with regards to time, I remember one of my mentors, Solomon Marcus, who I often evoke even though we’ve had completely different professions. When he turned 90 he asked me: “How long can a person live, doctor?” I wanted to give him an optimistic answer: “Let’s say 120 years, like in the Bible.” He told me: “That’s not enough for me, doctor, I have many projects!” So time isn’t friendly with any of us, especially when we have many projects and aren’t able to finish them and time goes by. After all, someone who is engaged on many fronts never has enough time.
Do you wish for anything special now, on the doorstep of your beautiful age?
Yes. Like any professor who has been a mentor for some generations of surgeons, my great wish is that they surpass the performances achieved by our generation. It’s something normal, because they will benefit from new technologies, new possibilities, a new type of medicine, imaging will be better, intensive care will be better, surgical means will be better – so I wish for them to carry on and perform at a higher level in Romanian surgery.
Thank you very much for your time, Professor, and I will reiterate my wish for you from the start of our meeting: Many happy returns!
Thank you very much. If you will allow me, as a last remark, I would take the liberty to express my great appreciation for what you are doing. It is the main reason why I was honoured to grant you this interview. I have been following your activity and I can say that few (somehow niche) journalists have proven such diligence over such a long period of time, such steadiness in their endeavours and a maximum strictness for this profession. I congratulate you for all you have done and wish you best of luck going forward.
Thank you very much, Professor. Coming from someone of your calibre, it means a lot to me. Thank you once again.
I wish you all the best!
Sursa / Source: https://youtu.be/ySI98U2V6Us




